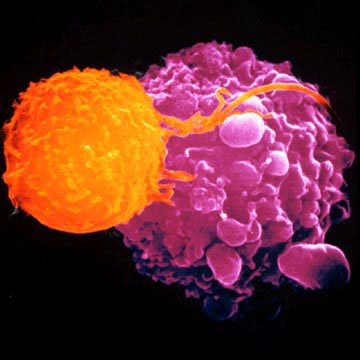
Vast numbers of cells that can attack cancer and HIV have been grown in the lab, and could potentially be used to fight disease.
The cells naturally occur in small numbers, but it is hoped injecting huge quantities back into a patient could turbo-charge the immune system.
The Japanese research is published in the journal Cell Stem Cell.
Experts said the results had exciting potential, but any therapy would need to be shown to be safe.
The researchers concentrated on a type of white blood cell known as a cytotoxic T-cell, which can recognize telltale markings of infection or cancer on the surfaces of cells. If a marking is recognized, it launches an attack.
Teams at the University of Tokyo and the Riken Research Centre for Allergy and Immunology used advances in stem cell technology to make more T-cells.
One group extracted T-cells which targeted a patient’s skin cancer. Another group did the same for HIV.
These T-cells were converted into stem cells, which could dramatically increase in number when grown in the laboratory. These were converted back into T-cells which should also have the ability to target the cancer or HIV.
The groups have proved only that they can make these cells, not that they can be safely put back into patients or that if would make a difference to their disease if they did.

Dr. Hiroshi Kawamoto, who worked on the cancer immune cells at Riken, said: “The next step will be to test whether these T-cells can selectively kill tumor cells, but not other cells in the body.
“If they do, these cells might be directly injected into patients for therapy. This could be realized in the not-so-distant future.”
Dr. Hiromitsu Nakauchi from the University of Tokyo said it was “unclear” whether this technique would help in treating HIV and that other infections and cancer may be a better place to start.
Experts in the field said the findings were encouraging.
Prof. Alan Clarke, the director of the European Cancer Stem Cell Research Institute at Cardiff University, said: “This is a potentially very exciting development which extends our capacity to develop novel cell therapies.”
He said it was important that cells could be tailored for each patient so there would be no risk of rejection.
Other experts said the findings were still at an early stage, but were still very promising and represented a strong foundation for future research. However, Cancer Research UK said it was still too early to know if any therapy would be safe.
Prof. Sir John Burn, from the Institute of Genetic Medicine at Newcastle University, said: “This is a very appealing concept and the research team are to be congratulated on demonstrating the feasibility of expanding these killer cells.”
However he added: “Even if these T cells are effective, it could prove very challenging to produce large quantities safely and economically.
“Nevertheless, there is real promise of this becoming an alternative when conventional therapies have failed.”